Dengue in Sri Lanka
District wise monthly Dengue cases – Jan 2022 to May 2023
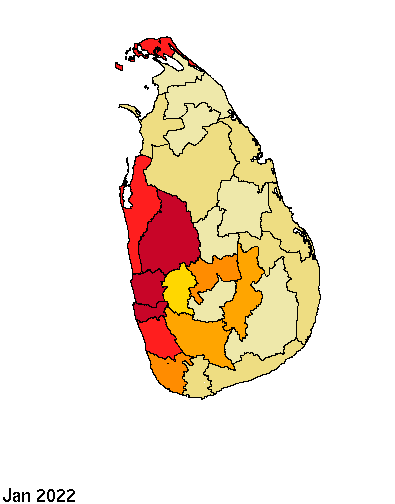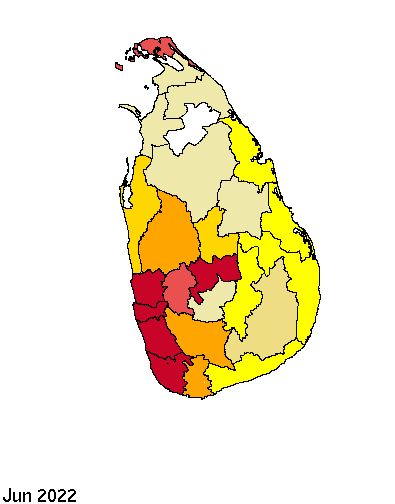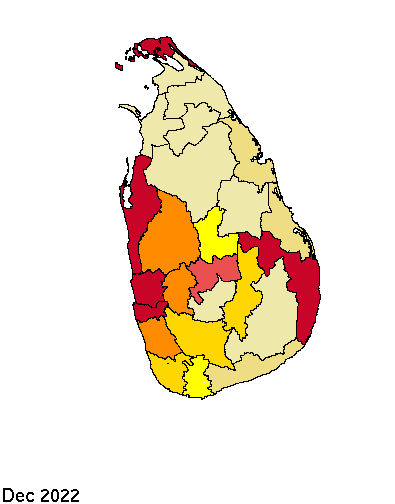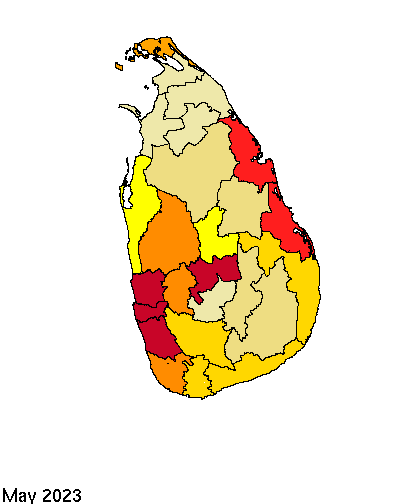

Overview
Dengue fever (DF) and dengue haemorrhagic fever (DHF) is an arbovirus disease transmitted by female mosquitoes of Aedes aegypti and Ae. albopictus. With its rapid expansion, Dengue has become a disease of global concern and a major threat. Dengue transmission is present in all the World Health Organization (WHO) regions and more than 125 countries are known to be dengue-endemic (Murray et al., 2013).
Dengue is mainly prevalent in Southeast Asia, Pacific and America and it is estimated worldwide, between 2.5 and 3.6 billion people which is over 50% of the population are at risk where urbanization and rapid population growth are also contributing factors (Ferriera, 2012; Guzman et al.,2010).
The lack of a vaccine means that control programs are reliant on management of environmental and human factors while the transmission cycle is also driven by fluctuations in climate, weather, quality of control programs and changes in dengue virology.
The impacts of Dengue are severe mainly affecting children and young adults causing large amount of fluid loss and in some cases dengue shock syndrome and fatalities in very serious circumstances (Hopp & Foley, 2001). Hence, disease severity and mortality are high. Dengue is highly intermittent, has some seasonality, and is showing an alarming exponential rise in the last few decades (Hopp & Foley, 2003).
Dengue has become the major public health problem in Sri Lanka in recent years. Dengue Fever (DF)/Dengue Hemorrhoid Fever (DHF) has become the major public health issue in urban and semi urban areas in Sri Lanka.
Over the past 27 years, morbidity, mortality and spatial distribution of disease have increased dramatically. In 2009 dengue reached 35007 DF/DHF cases and 346 deaths for 20 million population – the number of cases reached 184,442 in 2017. The rise is so dramatic so that high incidence year is like a disaster which impairs development. Early detection and predictions of the regions and periods with higher dengue risk shall help with the allocation of scarce public health resources.
Dengue in Sri Lanka
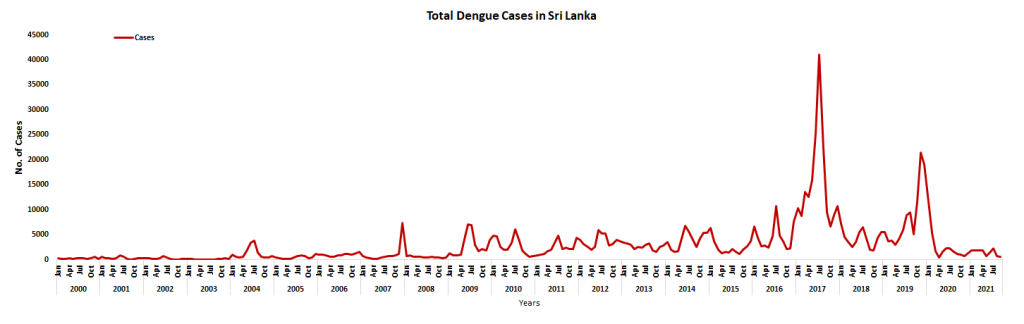
Globally, dengue is the fast-spreading arboviral disease and over 3.5 billion people, (over 40% of the world’s population) in more than 100 countries in the tropical and sub-tropical regions of the world are at risk of dengue transmission. In Sri Lanka, dengue was prevalent since the early 1960s, however, the disease became an important public health problem since early 2000s with the epidemic at 2 – 3-year intervals. Not only the number of dengue patients (cases), but the spatial distribution of cases was widened over the years.
Currently, dengue is endemic in Sri Lanka and patients are reported rural as well as rural areas of the country. The number of reported clinical and serologically positive dengue cases varied from 29,777 to 186,101 from 2010 – 2018 with the major epidemic in 2017 involving the 186,101 cases. (Epidemiological Unit, Sri Lanka, Dengue Reports). The sustained rise in dengue incidence is a current challenge which going by history is only going to be exacerbated in time.
The characterization of dengue has been reported in its early phases by Vitarana and others (1982, 1997) in Sri Lanka. Messer et al (2003) and De Silva et al (2005) has documented the introduction of new strains of dengue to Sri Lanka. The patterns of Dengue in Sri Lanka have changed mainly after 1989, where an exponential increase has been observed, involving high morbidity and mortality. Kularatne et al.,2006).
Dengue transmission involves humans, the dengue parasite, and mosquitoes which are referred to as the vector. Dengue prevention efforts include attempts at reducing the exposure of people to the vectors through bed-nets and screens, through eliminating mosquito breeding sites, through timely clean-up programs to early detection of dengue so as to eliminate the environmental factors leading to contracting the disease to save other people in the locality.
The rate of dengue transmission varies dramatically from place to place and time to time. Thus, having early warning of periods and places of higher risk in advance can help with focusing scarce resources as is typical in the tropics for control programs.
Dengue Vectors and Breeding Sites
In Sri Lanka, the primary and epidemic causing vector of DF/DHF is Aedes aegypti. Ae. albopictus is a secondary vector which causes epidemics when it occurs in high density (Kusumawathie et al., 2011). Both Aedes species are container breeders. Ae. aegypti prefers artificial containers and occurs more closely to the human habitations specially in urban and semi-urban areas. Ae. albopictus breeds in both artificial and natural container habitats (Kusumawathie and Fernando, 2003, Kusumawathie et al., 2007).
The common breeding sites are water storage tanks, barrels and discarded objects such as bottles, plastic items, tins, tyres; structures such as ponds, flowerpots and appliances such as refrigerator trays, cooking utensils (Kusumawathie and Siyambalagoda, 2005, Abeyewickreme et al., 2013). These types of breeding sites are found in every type of human dwelling in Sri Lanka (Kusumawathie 2005).
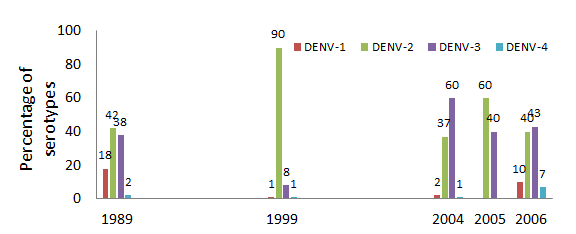
Change in Serotypes found in SL
There are four serotypes of dengue referred to as DENV-1, DENV-2, DENV-3, and DENV-4. If a patient acquires one of these types’ immunity, it follows that particular serotype only, but not against the others. These four serotypes have been circulating around Sri Lanka for almost three decades and in recent years changes have been noted where studies have shown changes in serotypes as well as different strains of the same serotype (Sirisena & Noordeen, 2014). A new genotype of DENV-1 serotype was introduced to Sri Lanka which was responsible for the 2009 epidemic for Dengue and DHF (Figure.) (Tissera et al., 2011). In addition, Messer et al. (2003), reported that the most severe form of the disease are persons infected with DENV-3 which has four geographically distinct different subtypes where Sri Lankan isolates were found to have subtype III.
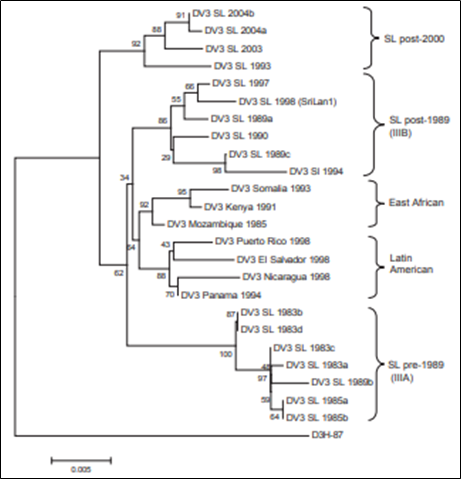
Many studies have been carried out to understand the immunological responses to dengue, as vaccine is yet to be discovered. In vitro studies carried out using mouse has shown alterations and changes in memory T lymphocytes which causes plasma leakage in DHF (Mathew and Rothman, 2008; Simmons et al, 2015; Duangchinda et al., 2010). Each serotype requires a different type of vaccine and some findings have proven the possibility of developing vaccines in the next few years, however a clear understanding of the pathogenesis of Dengue haemorrhagic fever/dengue shock syndrome is required (Beltramello et al., 2010; Halstead, 1980).
Application of timely and appropriate vector control interventions is the mainstay of disease prevention. Its prevalence in urban areas makes Asia particularly vulnerable and Sri Lanka one of the countries to be severely affected. In recent times, in Sri Lanka, dengue has transmission observed in semi-urban and rural areas and in estates in the central hill country. Due to population movement and travel, there has been the large-scale transmission of dengue Intra and inter-country and continent as mapped (Bhatt et al., 2013; Messer et al., 2003; De Silva et al., 2003).