MALARIA IN THE PAST
MALARIA IN THE PAST
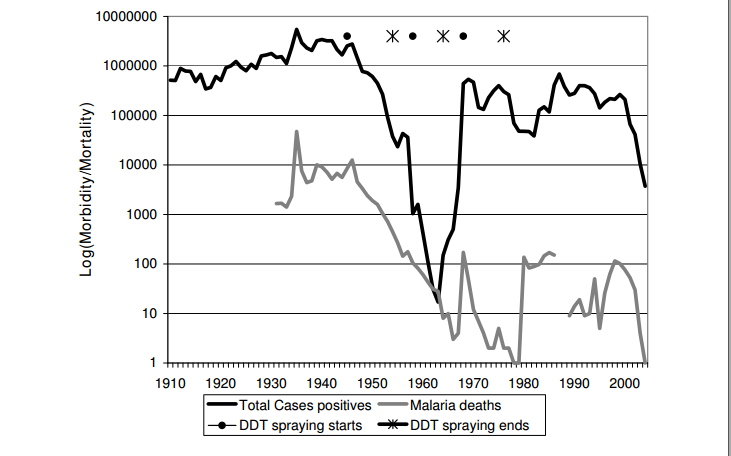
By the early 1900s, Malaria was well established in the country. Malaria in Sri Lanka in the past was a severe epidemic in the 1930s which led to an estimated 5.5 million cases and 80 000 deaths and near elimination of malaria during the Global Malaria Eradication Programme of the 1960s which reduced the number of cases from 91 000 in 1953 to a mere 17 in 1963 with many of these being imported cases.
As there was no continuous vigilance maintained and relaxed malaria control measures after the use of DDT there was a gradual increase in malaria incidence leading to island-wide epidemic with over 500,000 malaria cases being reported in 1969. The return of malaria led to a resumption of vector control measures, principally the indoor residual spraying of insecticides. There were only few deaths being reported as it was caused by the parasite P.vivax which is a less fatal parasite and P.falciparum for which there was treatment available in the country. The later years it was detected that DDT was resistance in An.culicifacies.
After the introductions of DDT, Malathione and other Anti Malaria substances Malaria was brought under control in the period after 1970s with few subsequent spikes. After reintroduction of new substances it curtailed and later in the past decade. Despite all this malaria resurged in 1999 and there were more than 200 000 reported cases of malaria. After the introduction of ACT in 2007 and other effective control measures in 2011 only 175 cases were reported a decrease of 99.9% compared to 1999. The Anti-Malaria campaign has been able to achieve a steady reduction in Malaria transmission rates and ultimately in 2012 indigenous malaria cases was completely eradicated.
(Source- Malaria free Sri Lanka, WHO Report 2016, Page 7-13 https://apps.who.int )
Anti Malaria Campaign, Ministry of Health, Nutrition and Indigenous Medicine, Sri Lanka AMC, History http://www.malariacampaign.gov.lk)
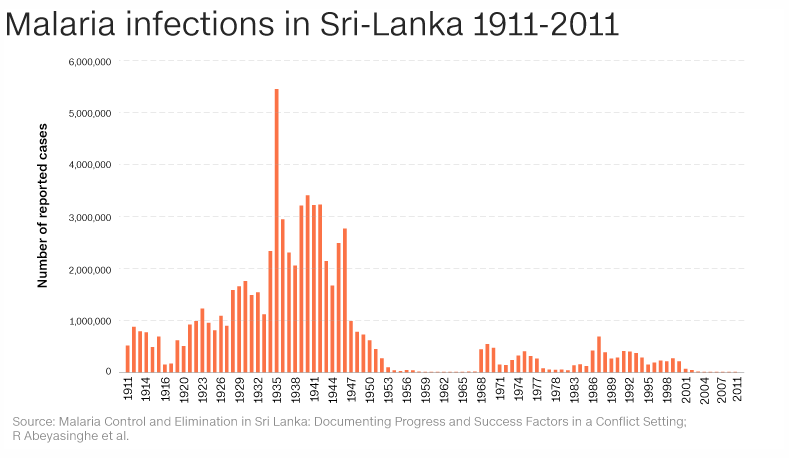
(Source – Malaria Control and Elimination in Sri Lanka)
HISTORY OF EPIDEMICS
The long history of malaria control in Sri Lanka offers a number of lessons for current malaria control services both in Sri Lanka and elsewhere. From 1868 to 1948 there have been 20 epidemics in Sri Lanka with case burdens reaching three million (60% of population) in the 1934–35 epidemic. Sri Lanka was remarkably successful during the “Global Malaria Eradication Campaign” reducing its burden from a typical two million cases per year in 1948 to just 17 cases in 1963. These control efforts included DDT-spraying and environmental measures such as anti-larval flushing of rivers. It appears that relaxation of control efforts around this time led to rapid and dramatic resurgence reaching 537,700 registered cases in 1969. Following this major epidemic, malaria control was revitalized and case numbers were brought down markedly, but another epidemic in 1975 produced 400,700 cases. Thereafter, there have been epidemics in 1983 (127,000), 1987(680,000 cases), 1991–2 (400,000 cases) and 1999 (290,000 cases). Presently Sri Lanka hosts 20 million people in a land area of 65,000 square kilometres. Plasmodium falciparum, which historically has been of low prevalence in comparison to Plasmodium vivax, has increased from 5% to above 25% of cases over the past few decades and is increasingly becoming resistant to the first-line anti-malarial drug, chloroquine. Recently malaria incidence has declined as Sri Lanka’s Anti-Malaria Campaign (AMC) has been implementing more effective malaria control activities. Since 2000 the incidence has reduced even further. Epidemics occur at three to five year intervals coinciding with low rainfall and high temperature, which favors the propagation of the vector Anopheles culicifacies sustained by secondary vectors such as Anopheles subpictus and Anopheles annularis. Malaria transmission in Sri Lanka is complex and vector breeding occurs in a range of settings, including: riverbeds, gem mining pits, seepage areas from irrigation reservoirs and canals and animal foot prints in moist regions, all with different ecological dynamics. The development of epidemic foci has been associated with slash and burn cultivation in poorly accessible deep forested areas, abandoned pits from gem mining areas and the migration of non-immune populations to endemic areas under resettlement programmes. These conditions occurred in late 1967 and 1968 prior to the 1969 epidemic.